

Journal of Surgery Concepts & Practice ›› 2025, Vol. 30 ›› Issue (04): 325-331.doi: 10.16139/j.1007-9610.2025.04.06
• Original article • Previous Articles Next Articles
HUANG Wenxin1, HE Qining1, Qi Debin1, Cao Zichao1, JIANG Yanzhi2a, WANG Pusen2b, QUE Weitao2b, ZHONG Lin1,2b( )
)
Received:2024-10-12
Online:2025-07-25
Published:2025-10-23
Contact:
ZHONG Lin
E-mail:zhonglin1@medmail.com.cn
CLC Number:
HUANG Wenxin, HE Qining, Qi Debin, Cao Zichao, JIANG Yanzhi, WANG Pusen, QUE Weitao, ZHONG Lin. Assessment of indocyanine green fluorescence imaging in hepatectomy for primary liver carcinoma: short-term prognostic analysis[J]. Journal of Surgery Concepts & Practice, 2025, 30(04): 325-331.
Tab 1
Comparison of preoperative general information between ICG and non-ICG groups[($\bar{x} \pm s$)/n(%)/M(Q1, Q3)]
| Item | ICG group (n=72) | non-ICG group (n=94) | t/χ²/Z value | P value |
|---|---|---|---|---|
| Age(years) | 61.9±12.3 | 58.8±11.2 | 1.703 | 0.091 |
| Gender | ||||
| Female | 17(23.6) | 30(31.9) | 1.385 | 0.239 |
| Male | 55(76.4) | 64(68.1) | ||
| HBsAg | ||||
| Negative | 34(47.2) | 33(35.1) | 2.486 | 0.115 |
| Positive | 38(52.8) | 61(64.9) | ||
| Preoperative examination | ||||
| Leukocyte(×109) | 5.5(4.2,7.7) | 5.47(4.6,6.4) | -0.370 | 0.711 |
| ALT(U/L) | 30.0(19.4,44.4) | 33.3(26.0,39.3) | -0.870 | 0.384 |
| AST(U/L) | 33.6(22.4,50.5) | 35.7(26.8,41.7) | -0.298 | 0.766 |
| AFP(μg/L) | 120.3(31.6,333.8) | 98.1(25.4,359.1) | -0.355 | 0.722 |
| Cirrhosis | ||||
| Negative | 37(51.4) | 46(48.9) | 0.098 | 0.754 |
| Positive | 35(48.6) | 48(51.1) | ||
| Child Pugh | ||||
| A | 68(94.4) | 89(94.7) | 0.004 | 0.947 |
| B | 4(5.6) | 5(5.3) | ||
| Tumor size (≥5 cm) | ||||
| Negative | 41(56.9) | 56(59.6) | 0.116 | 0.733 |
| Positive | 31(43.1) | 38(40.4) | ||
| Number of tumors | 1(1,1) | 1(1,1) | -0.74 | 0.941 |
| Degree of differentiation | ||||
| High | 11(15.3) | 9(9.6) | 1.290 | 0.525 |
| Moderate | 51(70.8) | 70(74.5) | ||
| Low | 10(13.9) | 15(16.0) | ||
| Tumor thrombus | ||||
| Negative | 66(91.7) | 90(95.7) | 1.198 | 0.274 |
| Positive | 6(8.3) | 4(4.3) | ||
| Tumor type | ||||
| Hepatocellular carcinoma | 48(66.7) | 67(71.3) | 0.422 | 0.810 |
| Intrahepatic bile duct carcinoma | 19(26.4) | 21(22.3) | ||
| Mixed liver carcinoma | 5(6.9) | 6(6.4) | ||
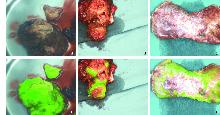
Fig 1
Gross observations and corresponding fluorescence pattern diagrams of liver tumor samples A: Gross view of fully fluorescent samples; B: Gross view of partially fluorescent samples; C: Gross view of circularly fluorescent samples; D: Fluorescence pattern of fully fluorescent samples; E: Fluorescence pattern of partially fluorescent samples; F: Fluorescence pattern of circularly fluorescent samples. The gross view (A-C) corresponded to the fluorescence pattern diagrams (D-F) as follows: A corresponds to D, B to E, and C to F.
Tab 2
Characteristics of different fluorescence types in the ICG group[n(%)]
| Item | Non-fluorescent (n=3) | Partially-fluorescent (n=32) | Circular-fluorescence (n=18) | Completely-fluorescent (n=19) | χ² value | P value |
|---|---|---|---|---|---|---|
| HBs Ag+ | 1(33.3) | 15(46.9) | 11(61.1) | 11(57.9) | 1.604 | 0.659 |
| HCV Ag+ | 0 | 1(3.1) | 0 | 1(5.3) | 1.049 | 0.789 |
| Cirrhosis | 0 | 18(56.3) | 4(22.2) | 13(68.4) | 17.875 | <0.001 |
| Tumor type | ||||||
| Hepatocellular carcinoma | 0 | 25(78.1) | 8(44.4) | 15(78.9) | 18.112 | 0.006 |
| Intrahepatic bile duct carcinoma | 3(100) | 4(12.5) | 9(50.0) | 3(15.8) | ||
| Mixed liver carcinoma | 0 | 3(9.4) | 1(5.6) | 1(5.3) | ||
| Degree of differentiation | ||||||
| High | 1(33.3) | 2(6.3) | 1(5.6) | 7(36.8) | 24.746 | <0.001 |
| Moderate | 1(33.3) | 28(87.5) | 10(55.6) | 12(63.2) | ||
| Low | 1(33.3) | 2(6.3) | 7(38.9) | 0 |
Tab 3
Comparison of intraoperative statistic in ICG and non-ICG groups[n(%)/M(Q1, Q3)]
| Item | ICG group (n=72) | non-ICG group (n=94) | χ²/Z value | P value |
|---|---|---|---|---|
| Operation time | 170(140,200) | 210(166,348) | -4.416 | <0.001 |
| Portal blockade rate | 7(9.7) | 31(33.0) | 12.493 | <0.001 |
| Intraoperative blood loss | 400(150,587.5) | 430(325,752.5) | -2.053 | 0.040 |
| Intraoperative blood transfusion rate | 14(19.4) | 21(22.3) | 0.206 | 0.650 |
Tab 4
Comparison of postoperative statistic in ICG and non-ICG groups[n(%)/M(Q1, Q3)]
| Item | ICG group(n=72) | non-ICG group (n=94) | χ²/Z value | P value |
|---|---|---|---|---|
| Surgical margin negative rate | 69(95.8%) | 86(91.5%) | 1.243 | 0.265 |
| Postoperative hospital stay | 10(8,12) | 14(10,21) | -4.317 | <0.001 |
| Number of painkillers used | 1(1,1) | 2(1,2) | -6.189 | <0.001 |
| Postoperative antibiotic use times | 1(1,1) | 2(1,2) | -5.738 | <0.001 |
| Drainage on the first day after surgery | 200(80,300) | 230(180,282.5) | -1.677 | 0.094 |
| The incidence of postoperative complications in the short term | 3(4.2) | 19(20.2) | 9.131 | 0.003 |
| Highest body temperature before discharge | 38(37.4,38.5) | 38.1(37.8,38.4) | -0.782 | 0.434 |
| Blood biochemistry on the first day after surgery | ||||
| Leukocyte(×109) | 11.6(8.5,16.0) | 14.3(12.5,16.3) | -3.680 | <0.001 |
| ALT(U/L) | 292.0(116.3,541.6) | 296.3(201.0,443.8) | -1.209 | 0.227 |
| AST(U/L) | 304.0(146.6,616.4) | 326.8(236.6,459.9) | -0.727 | 0.467 |
| TBil(μmol/L) | 23.5(18.1,29.7) | 27.0(18.2,33.6) | -1.060 | 0.289 |
| Albumin(g/L) | 34.6(30.4,37.0) | 31.4(29.3,33.6) | -3.611 | <0.001 |
| Blood biochemistry on the third day after surgery | ||||
| Leukocyte(×109) | 8.7(7.2,10.5) | 11.6(9.5,13.0) | -4.297 | <0.001 |
| ALT(U/L) | 180.8(100.5,504.5) | 193.4(143,265.3) | -1.267 | 0.205 |
| AST(U/L) | 94.9(55.8,270.2) | 124.5(84.2,168.5) | -2.042 | 0.041 |
| TBil(μmol/L) | 22.3(17.7,25.7) | 28.6(18.7,41.7) | -2.048 | 0.041 |
| Albumin(g/L) | 32.4(31.1,35.9) | 31.2(29.6,33.2) | -5.043 | <0.001 |
| Blood biochemistry on the seventh day after surgery | ||||
| Leukocyte(×109) | 8.8(6.2,10.0) | 7.7(6.4,9.4) | -1.069 | 0.285 |
| ALT(U/L) | 77.4(42.1,172.1) | 75.5(59.8,94.1) | -0.293 | 0.770 |
| AST(U/L) | 39.9(25.9,72.6) | 45.8(37.7,56.8) | -0.538 | 0.591 |
| TBil(μmol/L) | 19.6(15.8,23.9) | 22.3(14.9,32.9) | -1.396 | 0.163 |
| Albumin(g/L) | 34.4(31.0,36.5) | 32.8(30.9,34.9) | -1.785 | 0.074 |
| [1] |
RUMGAY H, ARNOLD M, FERLAY J, et al. Global burden of primary liver cancer in 2020 and predictions to 2040[J]. J Hepatol, 2022, 77(6):1598-1606.
doi: 10.1016/j.jhep.2022.08.021 pmid: 36208844 |
| [2] | SUNG H, FERLAY J, SIEGEL R L, et al. Global cancer statistics 2020:GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries[J]. CA Cancer J Clin, 2021, 71(3):209-249. |
| [3] | CHEN W, ZHENG R, BAADE P D, et al. Cancer statistics in China, 2015[J]. CA Cancer J Clin, 2016, 66(2):115-132. |
| [4] | European Association for the Study of the Liver. EASL clinical practice guidelines:management of hepatocellular carcinoma[J]. J Hepatol, 2018, 69(1):182-236. |
| [5] |
LLOVET J M, DE BAERE T, KULIK L, et al. Locoregional therapies in the era of molecular and immune treatments for hepatocellular carcinoma[J]. Nat Rev Gastroenterol Hepatol, 2021, 18(5):293-313.
doi: 10.1038/s41575-020-00395-0 pmid: 33510460 |
| [6] |
MAČIANSKIENĖ R, ALMANAITYTĖ M, TREINYS R, et al. Spectral characteristics of voltage-sensitive indocyanine green fluorescence in the heart[J]. Sci Rep, 2017, 7(1):7983.
doi: 10.1038/s41598-017-08168-7 pmid: 28801595 |
| [7] | EGLOFF-JURAS C, BEZDETNAYA L, DOLIVET G, et al. NIR fluorescence-guided tumor surgery:new strategies for the use of indocyanine green[J]. Int J Nanomedicine, 2019,14:7823-7838. |
| [8] |
KOKUDO N. Indocyanine green fluorescence imaging as an indispensable tool for modern liver surgery[J]. Ann Surg, 2022, 275(6):1035-1036.
doi: 10.1097/SLA.0000000000005425 pmid: 35185123 |
| [9] | 骆洋, 俞旻皓, 叶光耀, 等. 术中吲哚菁绿荧光显像评估在降低腹腔镜直肠癌术后吻合口漏的应用价值[J]. 外科理论与实践, 2023, 28(3):249-253. |
| LUO Y, YU M H, YE G Y, et al. Application value of intraoperative indocyanine green fluorescence imaging in reducing anastomotic leakage after laparoscopic rectal cancer surgery[J]. J Surg Concepts Pract, 2019, 28(3):249-253. | |
| [10] | CHEN Q Y, XIE J W, ZHONG Q, et al. Safety and efficacy of indocyanine green tracer-guided lymph node dissection during laparoscopic radical gastrectomy in patients with gastric cancer:a randomized clinical trial[J]. JAMA surgery, 2020, 155(4):300-311. |
| [11] |
WANG X, TEH C S C, ISHIZAWA T, et al. Consensus guidelines for the use of fluorescence imaging in hepatobiliary surgery[J]. Ann Surg, 2021, 274(1):97-106.
doi: 10.1097/SLA.0000000000004718 pmid: 33351457 |
| [12] | HSU A, MU S Z, JAMES A, et al. Indocyanine green in bariatric surgery:a systematic review[J]. Obes Surg, 2023, 33(11):3539-3544. |
| [13] | HAN H W, SHI N, ZOU Y P, et al. Functional anatomical hepatectomy guided by indocyanine green fluorescence imaging in patients with localized cholestasis:report of four cases[J]. World J Gastrointest Surg, 2021, 13(3):323-329. |
| [14] | ALFANO M S, MOLFINO S, BENEDICENTI S, et al. Intraoperative ICG-based imaging of liver neoplasms:a simple yet powerful tool. Preliminary results[J]. Surg Endosc, 2019, 33(1):126-134. |
| [15] | WAKABAYASHI T, CACCIAGUERRA A B, ABE Y, et al. Indocyanine green fluorescence navigation in liver surgery:a systematic review on dose and timing of administration[J]. Ann Surg, 2022, 275(6):1025-1034. |
| [16] |
SPERBER A D, BANGDIWALA S I, DROSSMAN D A, et al. Worldwide prevalence and burden of functional gastrointestinal disorders, results of rome foundation global study[J]. Gastroenterology, 2021, 160(1):99-114.e3.
doi: 10.1053/j.gastro.2020.04.014 pmid: 32294476 |
| [17] | LU C, RONG D, ZHANG B, et al. Current perspectives on the immunosuppressive tumor microenvironment in hepatocellular carcinoma:challenges and opportunities[J]. Mol Cancer, 2019, 18(1):130. |
| [18] |
DAI Y, QIANG W, LIN K, et al. An immune-related gene signature for predicting survival and immunotherapy efficacy in hepatocellular carcinoma[J]. Cancer Immunol Immunother, 2021, 70(4):967-979.
doi: 10.1007/s00262-020-02743-0 pmid: 33089373 |
| [19] | WATANABE J, TAKEMASA I, KOTAKE M, et al. Blood perfusion assessment by indocyanine green fluorescence imaging for minimally invasive rectal cancer surgery (EssentiAL trial):a randomized clinical trial[J]. Ann Surg, 2023, 278(4):e688-e694. |
| [20] |
DUROT I, WILSON S R, WILLMANN J K. Contrast-enhanced ultrasound of malignant liver lesions[J]. Abdom Radiol (NY), 2018, 43(4):819-847.
doi: 10.1007/s00261-017-1360-8 pmid: 29094174 |
| [21] |
NAKASEKO Y, ISHIZAWA T, SAIURA A. Fluorescence-guided surgery for liver tumors[J]. J Surg Oncol, 2018, 118(2):324-331.
doi: 10.1002/jso.25128 pmid: 30098296 |
| [22] |
CASSINOTTI E, AL-TAHER M, ANTONIOU S A, et al. European association for endoscopic surgery (EAES) consensus on indocyanine green (ICG) fluorescence-guided surgery[J]. Surg Endosc, 2023, 37(3):1629-1648.
doi: 10.1007/s00464-023-09928-5 pmid: 36781468 |
| [23] | TANG Y, HUANG Z, ZHANG X, et al. Effect of visceral obesity on outcomes of fluorescence-guided lymphadenectomy during laparoscopic gastrectomy for gastric cancer:Post hoc analysis of a randomized phase 3 trial[J]. Chin J Cancer Res, 2024, 36(5):503-516. |
| [24] | CHEN Q Y, ZHONG Q, LIU Z Y, et al. Indocyanine green fluorescence imaging-guided versus conventional laparoscopic lymphadenectomy for gastric cancer:long-term outcomes of a phase 3 randomised clinical trial[J]. Nat Commun, 2023, 14(1):7413. |
| [25] | 周煦川, 刘宾, 王文飞, 等. 多点注射吲哚菁绿红外显影在下肢淋巴管-静脉吻合术中的应用[J]. 组织工程与重建外科杂志, 2023, 19(5):459-463 |
| ZHOU X C, LIU B, WANG W F, et al. Application of multi-point injection of indocyanine green infrared imaging in lymphangio-venous anastomosis of lower extremities[J]. J Tissue Eng Reconstr Surg, 2019, 19(5):459-463. | |
| [26] | RUZZENENTE A, CONCI S, ISA G, et al. The LIver SEntinel LYmph-node (LISELY) study:a prospective intraoperative real time evaluation of liver lymphatic drainage and sentinel lymph-node using near-infrared (NIR) imaging with indocyanine green (ICG)[J]. Eur J Surg Oncol, 2022, 48(12):2455-2459. |
| [27] | WU M R, HUANG Y Y, HSIAO J K. Use of indocyanine green (ICG), a medical near infrared dye, for enhanced fluorescent imaging-comparison of organic anion transporting polypeptide 1B3 (OATP1B3) and sodium-taurocholate cotransporting polypeptide (NTCP) reporter genes[J]. Molecules, 2019, 24(12):2295. |
| [28] | ANZAI K, TSURUYA K, MORIMACHI M, et al. The impact of a heterozygous SLCO1B3 null variant on the indocyanine green retention test[J]. J Pharm Sci, 2020, 109(10):3206-3209. |
| [29] | ISHIZAWA T, SAIURA A, KOKUDO N. Clinical application of indocyanine green-fluorescence imaging during hepatectomy[J]. Hepatobiliary Surg Nutr, 2016, 5(4):322-328. |
| [30] | FENG H L, LI Q, WANG L, et al. Indocyanine green clearance test combined with MELD score in predicting the short-term prognosis of patients with acute liver fai-lure[J]. Hepatobiliary Pancreat Dis Int, 2014, 13(3):271-275. |
| [1] | LU Zhiyu, SUN Ji, DU Jialu, MENG Xuan, LUO Man, LIU Yue, WANG Hongguang. Research on the management of the Glissonean pedicle in laparoscopic anatomical hemihepatectomy and the influence of indocyanine green dose on the fluorescence staining effect [J]. Journal of Surgery Concepts & Practice, 2024, 29(02): 138-142. |
| [2] | LI Shule, LU Lu. Development and prospect of laparoscopic living donor hepatectomy [J]. Journal of Surgery Concepts & Practice, 2024, 29(02): 121-125. |
| [3] | HOU Zhenyu, KONG Yinlong, ZHANG Yongqiang, ZHU Keyun, YANG Xuejiao, CHEN Ping, LI Huikai, CUI Yunlong, SONG Tianqiang, LI Qiang, ZHANG Ti. Preoperative white blood cell count predicts prognosis in patients with hepatocellular carcinoma beyond Milan criteria after hepatic resection [J]. Journal of Surgery Concepts & Practice, 2018, 23(04): 358-362. |
| [4] | ZHANG Yongqiang, ZHANG Ti, KONG Yinlong, HOU Zhenyu, LI Huikai, CUI Yunlong, SONG Tianqiang, LI Qiang. Intraoperative hemorrhage related to perioperative events and prognosis of patients with early stage hepatocellular carcinoma [J]. Journal of Surgery Concepts & Practice, 2018, 23(04): 342-345. |
| [5] | JIN Shengjie, FAN Yiqun, BAI Dousheng, JIANG Guoqing, QIAN Jianjun, YAO Jie, WANG Xiaodong, GAO Zhihui, ZHANG Chi. Experience of portal vein embolization for two-stage precise hepatectomy [J]. Journal of Surgery Concepts & Practice, 2018, 23(03): 247-251. |
| [6] | . [J]. Journal of Surgery Concepts & Practice, 2014, 19(06): 529-534. |
| [7] | . [J]. Journal of Surgery Concepts & Practice, 2014, 19(05): 459-463. |
| [8] | . [J]. Journal of Surgery Concepts & Practice, 2013, 18(02): 125-130. |
| [9] | . [J]. Journal of Surgery Concepts & Practice, 2012, 17(05): 437-443. |
| [10] | . [J]. Journal of Surgery Concepts & Practice, 2011, 16(06): 526-530. |
| [11] | . [J]. Journal of Surgery Concepts & Practice, 2010, 15(04): 369-374. |
| [12] | . [J]. Journal of Surgery Concepts & Practice, 2009, 14(01): 28-32. |
| [13] | . [J]. Journal of Surgery Concepts & Practice, 2008, 13(04): 316-321. |
| [14] | . [J]. Journal of Surgery Concepts & Practice, 2008, 13(03): 220-222. |
| [15] | . [J]. Journal of Surgery Concepts & Practice, 2005, 10(04): 323-328. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||