

Journal of Surgery Concepts & Practice ›› 2023, Vol. 28 ›› Issue (06): 556-562.doi: 10.16139/j.1007-9610.2023.06.012
• Original article • Previous Articles Next Articles
FENG Meijing1, REN Xinping1,2( ), ZHAN Weiwei1,2, ZHENG Lili1, LI Junjian1
), ZHAN Weiwei1,2, ZHENG Lili1, LI Junjian1
Received:2022-10-08
Online:2023-11-25
Published:2024-03-04
CLC Number:
FENG Meijing, REN Xinping, ZHAN Weiwei, ZHENG Lili, LI Junjian. Value of contrast-enhanced ultrasound in differentiating benign and malignant gallbladder lesions which diameter more than 1 cm[J]. Journal of Surgery Concepts & Practice, 2023, 28(06): 556-562.
Tab 1
General characteristics of benign group and malignant group gallbladder lesions [M(IQR)/n(%)]
| Characteristics | Malignant lesions (n=43) | Benign lesions (n=99) | Test statistic value | P value |
|---|---|---|---|---|
| Gross type (n/%) | χ2=56.480 | <0.001 | ||
| Mass type | 9(20.9) | 85(85.9) | ||
| Thick-walled type | 34(79.1) | 14(14.1) | ||
| Characteristic | ||||
| Diameter (mm) M(IQR) | 32.0(20.0) | 15.5(14.0) | Z=5.522 | <0.001 |
| Quantity (n/%) | χ2=15.089 | <0.001 | ||
| Single shot | 29(67.4) | 32(32.3) | ||
| Multiple | 14(32.6) | 67(67.7) | ||
| Form(n/%) | χ2=36.776 | <0.001 | ||
| Rule | 12(27.9) | 80(80.8) | ||
| Irregularity | 31(72.1) | 19(19.2) | ||
| Echo (n/%) | χ2=14.529 | 0.002 | ||
| Hyperechoic | 12(27.9) | 49(49.5)a) | ||
| Hypoechoic | 10(23.3) | 4(4.0) a) | ||
| Isoechoic | 14(32.6) | 30(30.3) | ||
| Mixed echoic | 7(16.3) | 16(16.2) | ||
| Gallbladder wall (n/%) | χ2=0.320 | 0.572 | ||
| Thickening | 16(37.2) | 32(32.3) | ||
| No thickening | 27(62.8) | 67(67.7) | ||
| Gallbladder and liver boundary (n/%) | χ2=38.523 | <0.001 | ||
| Clear | 21(48.8) | 93(93.9) | ||
| Unclear | 22(51.2) | 6(6.1) | ||
| Gallstone (n/%) | 0.553 | |||
| Yes | 3(7.0) | 12(12.1) | ||
| No | 40(93.0) | 87(87.9) |
Tab 2
CEUS characteristics of gallbladder lesions in benign group and malignant group [M(IQR)/n(%)]
| Characteristics of CEUS | Malignant lesions (n=43) | Benign lesions (n=87) | Test statistic value | P value |
|---|---|---|---|---|
| Enhancement patterns (n/%) | χ2=30.658 | <0.001 | ||
| Homogeneously | 8(18.6) | 61(70.1) | ||
| Heterogeneously | 35(81.4) | 26(29.9) | ||
| Enhancement level (n/%) | χ2=22.132 | <0.001 | ||
| Hyperenhancement | 33(76.8) | 30(34.5)a) | ||
| Isoenhancement | 5(11.6) | 14(16.1) | ||
| Hypo-enhancement | 5(11.6) | 43(49.4)a) | ||
| Contrast arrival time(s) M(IQR) | 15(6) | 18(6) | Z=10.753 | <0.001 |
| Contrast washout time(s) M(IQR) | 45(29) | 64(40) | Z=3.794 | <0.001 |
| Wall continuity (n/%) | χ2=41.611 | <0.001 | ||
| Continuity | 18(41.9) | 81(93.1) | ||
| Discontinuity | 25(58.1) | 6(6.8) |
Fig 1
Conventional ultrasound and CEUS images of a patient with gallbladder adenocarcinoma (female, 66 years old) A: Conventional ultrasound showed multiple strong echoes in the gallbladder, followed by sound shadow, and flaky hypoechoic echoes. No blood flow signal was detected in the hypoechoic echoes;B: CEUS showed thickening of the gallbladder wall at the base of the gallbladder, rapid high enhancement at the arterial phase, reaching peak at 15 s, perfusion intensity higher than the surrounding gallbladder wall; C: Subsided to low enhancement in 28 s.
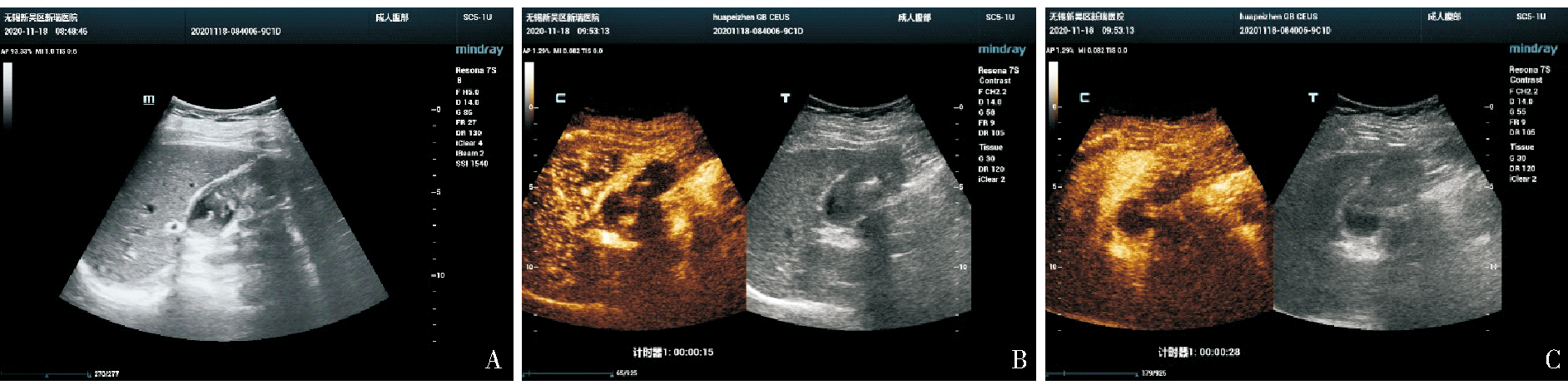
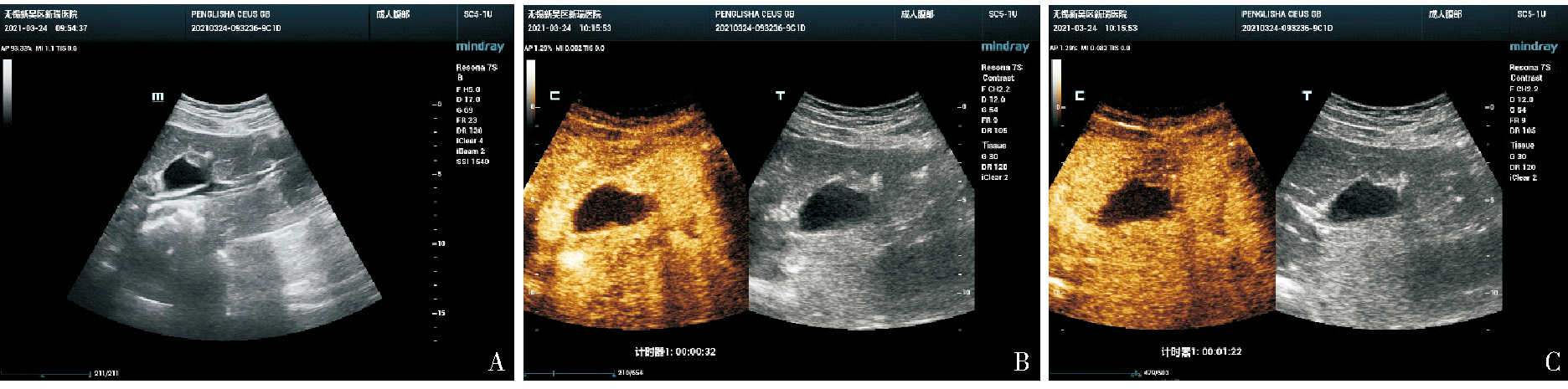
Fig 2
Conventional ultrasound and CEUS images of a patient with gallbladder adenomyosis (female, 32 years old) A: Conventional ultrasound showed solid hypoechoic area at the base of the gallbladder (white arrow) with uniform internal echo, and no detectable blood flow signal; B: CEUS showed that the hypoechoic mass in the base of the gallbladder peaked in 22 s, and the perfusion intensity was similar to that of the gallbladder wall, with good continuity in the gallbladder wall; C: Showed a low enhancement at 1 m 22 s in venous phase.
Tab 3
Comparison the three diagnostic methods with the gold standard (n)
| Gold standard | CEUS standard | CEUS standard combined with contrast medium washout before 60 s | CEUS standard combined with contrast medium washout before 35 s | |||||
|---|---|---|---|---|---|---|---|---|
| Malignant | Benign | Malignant | Benign | Malignant | Benign | |||
| Malignant | 40 | 3 | 42 | 1 | 40 | 3 | ||
| Benign | 16 | 83 | 40 | 59 | 7 | 92 | ||
| κ value | 0.708 | 0.456 | 0.837 | |||||
Tab 4
Diagnostic efficacy of three diagnostic methods (%)
| Diagnostic effectiveness | CEUS standard | CEUS standard combined with contrast medium washout before 60 s | CEUS standard combined with contrast medium washout before 35 s |
|---|---|---|---|
| Sensitivity | 93.0 | 97.7 | 93.0 |
| Specificity | 83.8 | 59.6 | 92.9 |
| Positive predictive value | 71.4 | 51.2 | 85.1 |
| Negative predictive value | 96.5 | 98.3 | 96.8 |
| Accuracy | 86.6 | 71.1 | 93.0 |
| [1] |
WENNMACKER S Z, DE SAVORNIN LOHMAN E A J, HASAMI N A, et al. Overtreatment of nonneoplastic gallbladder polyps due to inadequate routine ultrasound assessment[J]. Dig Surg, 2020, 10:1-7.
doi: 10.1159/000172129 URL |
| [2] |
WENNMACKER S Z, VAN DIJK A H, RAESSENS J H J, et al. Polyp size of 1cm is insufficient to discriminate neoplastic and non-neoplastic gallbladder polyps[J]. Surg Endosc, 2019, 33(5):1564-1571.
doi: 10.1007/s00464-018-6444-1 |
| [3] |
KAMAYA A, FUNG C, SZPAKOWSKI J L, et al. Management of incidentally detected gallbladder polyps: society of radiologists in ultrasound consensus conference recommendations[J]. Radiology, 2022, 305(2):277-289.
doi: 10.1148/radiol.213079 URL |
| [4] | 史艳平, 张秀秀, 樊文文, 等. 超声造影与增强CT诊断胆囊占位性病变的对比研究[J]. 临床超声医学杂志, 2019, 21(11):841-844. |
| SHI Y P, ZHANG X X, FAN W W, et al. Comparative study of contrast-enhanced ultrasound and enhanced CT in gallbladder space-occupying lesions[J]. J Clin Ultrasound in Med, 2019, 21(11):841-844. | |
| [5] |
SIDHU P S, CANTISANI V, DIETRICH C F, et al. The EFSUMB guidelines and recommendations for the clinical practice of contrast-enhanced ultrasound (CEUS) in non-hepatic applications: update 2017 (long version)[J]. Ultraschall Med, 2018, 39(2):e2-e44.
doi: 10.1055/a-0586-1107 URL |
| [6] |
SERRA C, FELICANI C, MAZZOTTA E, et al. CEUS in the differential diagnosis between biliary sludge, benign lesions and malignant lesions[J]. J Ultrasound, 2018, 21(2):119-126.
doi: 10.1007/s40477-018-0286-5 pmid: 29476456 |
| [7] |
WANG W, FEI Y, WANG F. Meta-analysis of contrast-enhanced ultrasonography for the detection of gallbladder carcinoma[J]. Med Ultrason, 2016, 18(3):281-288.
doi: 10.11152/mu.2013.2066.183.wei pmid: 27622402 |
| [8] | 中国医师协会超声医师分会. 中国超声造影临床应用指南[M]. 北京: 人民卫生出版社, 2017. |
| Sonographer Branch of Chinese Medical Doctor Association. Chinese guidelines for clinical application of contrast-enhanced ultrasound[M]. Beijing: People's Medical Publishing House, 2017. | |
| [9] |
ZHANG H P, BAI M, GU J Y, et al. Value of contrast-enhanced ultrasound in the differential diagnosis of gallbladder lesion[J]. World J Gastroenterol, 2018, 24:744-751.
doi: 10.3748/wjg.v24.i6.744 URL |
| [10] | ZHUANG B, LI W, WANG W, et al. Contrast-enhanced ultrasonography improves the diagnostic specificity for gallbladder-confined focal tumors[J]. Abdom Radiol(NY), 2018, 43:1134-1142. |
| [11] | CHEN L D, HUANG Y, XIE X H, et al. Diagnostic nomogram for gallbladder wall thickening mimicking malignancy: using contrast-enhanced ultrasonography or multi-detector com-puted tomography?[J]. Abdom Radiol(NY), 2017, 42:2436-2446. |
| [12] | 费翔, 罗渝昆. 胆囊超声造影指南解读与图像分析[J]. 中华医学超声杂志(电子版), 2018, 15(1):5-9. |
| FEI X, LUO Y K. Interpretation and image analysis of gallbladder contrast-enhanced ultrasound guidelines[J]. Chin J Med Ultrasound (electronic edition), 2018, 15(1):5-9. | |
| [13] | 吴少虹, 程美清, 谢晓燕, 等. 胆囊癌超声造影特征分析[J]. 临床超声医学杂志, 2018, 20(12):842-845. |
| WU S H, CHENG M Q, XIE X Y, et al. The characteristics of contrast-enhanced ultrasound of gallbladder carcinoma[J]. Clin Ultrasound in Med, 2018, 20(12):842-845. | |
| [14] |
LIU L N, XU H X, LU M D, et al. Contrast-enhanced ultrasound in the diagnosis of gallbladder diseases: a multi-center experience[J]. PLoS One, 2012, 7(10):e48371.
doi: 10.1371/journal.pone.0048371 URL |
| [15] |
YUAN H X, CAO J Y, KONG W T, et al. Contrast-enhanced ultrasound in diagnosis of gallbladder adenoma[J]. Hepatobiliary Pancreat Dis Int, 2015, 14(2):201-207.
doi: 10.1016/S1499-3872(15)60351-4 URL |
| [16] |
FEI X, LU W P, LUO Y K, et al. Contrast-enhanced ultrasound may distinguish gallbladder adenoma from cholesterol polyps: a prospective case-control study[J]. Abdom Imaging, 2015, 40(7):2355-2363.
doi: 10.1007/s00261-015-0485-x pmid: 26082060 |
| [17] | 郑茹瑜, 丁建民, 周燕, 等. 超声造影在诊断厚壁型胆囊癌中的应用[J]. 中国医学影像学杂志, 2020, 28(3):210-214. |
| ZHENG R Y, DING J M, ZHOU Y, et al. Contrast-enhanced ultrasound in the diagnosis of thick-walled gallbladder carcinoma[J]. Chin J Medical Imaging, 2020, 28(3):210-214. | |
| [18] | CHENG Y, WANG M, MA B, et al. Potential role of contrast-enhanced ultrasound for the differentiation of malignant and benign gallbladder lesions in East Asia: a meta-analysis and systematic review[J]. Medicine(Baltimore), 2018, 97(33):e11808. |
| [19] |
KONG W T, SHEN H Y, QIU Y D, et al. Application of contrast enhanced ultrasound in gallbladder lesion: is it helpful to improve the diagnostic capabilities?[J]. Med Ultrason, 2018, 20(4):420-426.
doi: 10.11152/mu-1626 URL |
| [20] |
NEGRÃO DE FIGUEIREDO G, MUELLER-PELTZER K, ZENGEL P, et al. Contrast-enhanced ultrasound (CEUS) and gallbladder diseases - a retrospective mono-center analysis of imaging findings with histopathological correlation[J]. Clin Hemorheol Microcirc, 2019, 71(2):151-158.
doi: 10.3233/CH-189405 pmid: 30584127 |
| [21] |
XIE X H, XU H X, XIE X Y, et al. Differential diagnosis between benign and malignant gallbladder diseases with real-time contrast-enhanced ultrasound[J]. Eur Radiol, 2010, 20(1):239-248.
doi: 10.1007/s00330-009-1538-8 URL |
| [22] | 苗燕, 张炎晶, 刘利平, 等. 裸鼠胆囊癌皮下移植瘤超声造影定量参数与血管生成及细胞增殖的相关性[J]. 中国医学影像技术, 2017, 33(6):822-825. |
| MIAO Y, ZHANG Y J, LIU L P, et al. Correlation between CEUS parameters and angiogenesis and cell proliferation of gallbladder carcinoma transplant tumor in nude mice[J]. Chin J Med Imaging Technol, 2017, 33(6):822-825. |
| [1] | LI Xiaoshi, QIN Yue. Multiple radiology imaging techniques in the diagnosis of gout [J]. Journal of Diagnostics Concepts & Practice, 2023, 22(03): 311-318. |
| [2] | YANG Qiao, FU Xin, WANG Zhe, LIU Tantan. Cytopathologic analysis of thyroid secondary tumors [J]. Journal of Diagnostics Concepts & Practice, 2023, 22(03): 270-276. |
| [3] | WU Nanming, LI Jun, TAO Juan. Hot spots in diagnosis of malignant melanoma [J]. Journal of Diagnostics Concepts & Practice, 2023, 22(03): 215-220. |
| [4] | WANG Yuanjiang, ZOU Hao. Clinical study on comprehensive treatment of gallbladder cancer [J]. Journal of Surgery Concepts & Practice, 2023, 28(02): 171-176. |
| [5] | XING Ying, CHENG Shi. Neoadjuvant therapy for gallbladder cancer: current status and challenge [J]. Journal of Surgery Concepts & Practice, 2023, 28(02): 110-114. |
| [6] | XIE Yaqiong, LIN Xiaoyi. Value of serum-free light chain assay in differential diagnosis and staging of nephropathy of various etiologies [J]. Journal of Diagnostics Concepts & Practice, 2023, 22(02): 166-171. |
| [7] | HAO Jiaqi, WANG Xinlu, HU Xiaofan, PAN Xiaoxia, XU Jing, MA Jun. Clinical differential diagnosis of acute tubulointerstitial nephritis and acute tubular necrosis [J]. Journal of Diagnostics Concepts & Practice, 2023, 22(02): 127-133. |
| [8] | FENG Meijing, REN Xinping. Application of contrast-enhanced ultrasound in diagnosis of gallbladder protrusion lesions [J]. Journal of Diagnostics Concepts & Practice, 2023, 22(01): 68-74. |
| [9] | REN Xinping, LI Junjian, ZHANG Jie, ZHAN Weiwei. Advances in the application of contrast-enhanced ultrasound in the diagnosis and treatment of focal liver lesions [J]. Journal of Diagnostics Concepts & Practice, 2022, 21(06): 684-690. |
| [10] | LIU Miao, SHEN Yan, FU Xiaohong, HU Jiaojiao, CHEN Qingqing, YING Tao. A comparative study on breast cancer between smaller and larger diameters using conventional ultrasound and contrast-enhanced ultrasound [J]. Journal of Surgery Concepts & Practice, 2022, 27(03): 229-233. |
| [11] | WANG Zhaohui, WU Haibo. Clinicopathological analysis of 31 cases of gastric schwannoma [J]. Journal of Diagnostics Concepts & Practice, 2021, 20(06): 552-556. |
| [12] | ZHANG Daojian, ZHANG Dexiang, WANG Jiwen, LU Pinxiang, LIU Houbao, LIU Han. Contrast-enhanced ultrasound in differential diagnosis of gallbladder cancer from xanthogranulomatous cholecystitis [J]. Journal of Surgery Concepts & Practice, 2020, 25(04): 322-325. |
| [13] | WANG Jianjun, CHEN Ya, FAN Xiangshan, NIU Fengnan. Sclerosing angiomatoid nodular transformation of spleen: clinicopathological analysis and literature review [J]. Journal of Diagnostics Concepts & Practice, 2019, 18(05): 560-564. |
| [14] | CHANG Rui, XU Jiaxu, DONG Haipeng, WU Mengxiong, ZHAO Xuesong, MIAO Fei, YAN Fuhua. Value of CT spectral imaging in the evaluation of Crohn's disease activity [J]. Journal of Diagnostics Concepts & Practice, 2019, 18(04): 432-435. |
| [15] | YANG Ruxue, LI Nan, ZHOU Ting, ZHAO Yan, CHEN Shaohua, ZHU Qing, FENG Zhenzhong. Clinicopathologic analysis of skin melanocyte lesions [J]. Journal of Diagnostics Concepts & Practice, 2018, 17(05): 566-571. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||